Postpartum Pelvic Floor Recovery Workouts For Women

Recovering from childbirth while your body faces the natural changes that come with being over 40 can be really challenging.
The slower healing, declining estrogen levels, and muscle loss that accelerates after 40 aren’t just statistics—they’re your daily reality as you change diapers, lift your baby, and wonder if you’ll ever feel like yourself again.
Let’s talk about what nobody mentions in those glossy postpartum recovery posts: the leaking when you cough, the heaviness you feel by afternoon, the fear that intimacy might never feel comfortable again.
You’re not broken. You’re experiencing pelvic floor dysfunction, and it affects up to 50% of women after childbirth—even more common when you’re over 40.
Here’s what you need to know right now: science-backed exercises performed consistently for just 12-25 minutes daily can transform your pelvic floor strength in 6-12 weeks.
This isn’t about “bouncing back” to some unrealistic standard. This is about building back stronger, with the wisdom and patience that younger moms haven’t developed yet.
You’re about to discover the proven exercises that rebuild your pelvic floor from the foundation up, a realistic timeline for recovery, and why your age is actually an advantage when you approach this journey with intention. It’s never too late to reclaim your pelvic health and feel powerful in your body again.
Why Pelvic Floor Recovery Looks Different After 40

The Biology Behind the Challenge
Your body operates under different rules now. Declining estrogen levels directly affect tissue elasticity and healing speed—the same hormones that kept your muscles and connective tissues resilient are decreasing. Research shows that sarcopenia (muscle mass loss) accelerates after 40, reducing muscle by 3-8% per decade. Your pelvic floor muscles aren’t exempt from this process.
Collagen production decreases by about 1% each year after your mid-twenties, impacting how quickly connective tissue repairs itself. When you combine pregnancy’s physical demands with age-related tissue changes, recovery takes longer and requires more strategic effort.
This isn’t about your body failing you. Understanding these biological realities helps you set appropriate expectations and choose effective strategies. You’re not trying to reverse time—you’re working with your body’s current capabilities to build genuine, lasting strength.
Common Symptoms You Shouldn’t Ignore
Stress incontinence shows up during exercise, coughing, sneezing, or laughing—those unexpected leaks that make you plan your life around bathroom locations. You might feel heaviness or bulging sensations that signal pelvic organ prolapse, where weakened muscles allow organs to shift downward.
Lower back pain and hip instability often accompany pelvic floor dysfunction because these muscle groups work together. When your pelvic floor can’t provide adequate support, your back and hips compensate, creating pain patterns that interfere with daily activities.
Painful intercourse or reduced sensation affects your relationship and confidence. Diastasis recti—the separation of abdominal muscles—compounds pelvic floor issues, creating a cascade of core weakness that impacts everything from posture to breathing.
These symptoms are common, but they’re not inevitable or permanent. Recognizing them is the first step toward effective recovery.
The Good News: Your Body Is Incredibly Adaptable
Research demonstrates that effective pelvic floor recovery is possible at any age. A 2019 study in the International Urogynecology Journal found that women who performed targeted pelvic floor exercises showed significant improvement regardless of age, with consistent practice producing measurable results in 6-12 weeks.
If you’ve exercised before pregnancy, muscle memory works in your favor. Your neuromuscular pathways remember movement patterns, making it easier to reconnect with your pelvic floor and rebuild strength efficiently.
You bring something younger moms often lack: wisdom, patience, and commitment. You understand that sustainable results require consistency over intensity. You’re less likely to push through pain or ignore warning signs. Your maturity is a powerful asset in this recovery journey.
The Foundation: Understanding Your Pelvic Floor
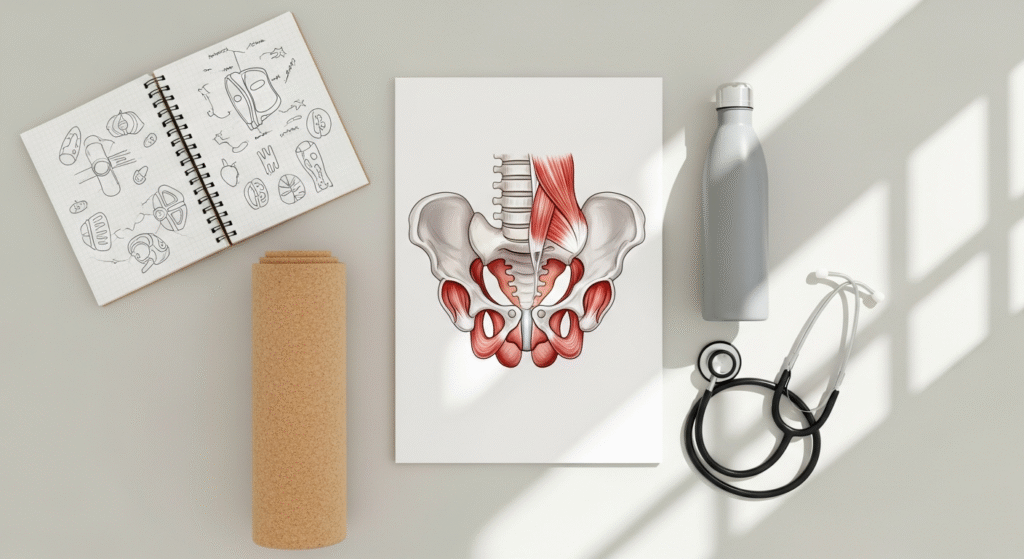
What Your Pelvic Floor Actually Does
Think of your pelvic floor as a hammock of muscles stretching from your pubic bone to your tailbone, supporting your bladder, uterus, and bowel. These powerful muscles control urination and bowel movements, support your organs against gravity, and contribute to sexual function and core stability.
Pregnancy stretches these muscles as your baby grows, and childbirth—whether vaginal or cesarean—creates trauma that weakens their structure. A vaginal delivery can stretch pelvic floor muscles to three times their normal length. Even a C-section affects these muscles because pregnancy itself changes their function.
Your pelvic floor doesn’t work in isolation. It’s intimately connected to your deep core muscles, diaphragm, and back muscles. When one component weakens, the entire system compensates, creating dysfunction that extends beyond your pelvis. This is why comprehensive recovery addresses breathing, posture, and core strength alongside targeted pelvic floor work.
The Breath-Core-Pelvic Floor Connection
Your diaphragm and pelvic floor move together with each breath. When you inhale, your diaphragm descends and your pelvic floor gently releases. When you exhale, both rise back up. This coordinated movement is essential for proper pelvic floor function.
Diaphragmatic breathing—deep belly breathing—activates your pelvic floor muscles naturally. The transverse abdominis, your deepest core muscle, wraps around your torso like a corset and works with your pelvic floor to stabilize your spine and pelvis during movement.
Many women fall into the “squeeze and hold” trap, constantly gripping their pelvic floor muscles. This creates tension and dysfunction rather than strength. Effective pelvic floor recovery requires coordination—learning when to engage, when to release, and how to integrate these muscles into functional movement patterns.
Signs Your Pelvic Floor Is Healing
You’ll notice reduced leakage incidents first—fewer accidents during exercise or when you sneeze. Your posture improves naturally as core stability returns. The heaviness or pressure you felt by afternoon diminishes, and you can stand or walk longer without discomfort.
Bladder control improves gradually. You’ll experience fewer urgent bathroom trips and greater confidence during daily activities. You might notice that you can hold your baby longer without back pain or that lifting feels more stable and controlled.
These improvements build on each other. Small wins compound into significant functional changes that transform your daily life and confidence.
Before You Start: Essential Safety Guidelines

Get Medical Clearance First
Most healthcare providers clear women for exercise at 6-8 weeks postpartum, but this timeline varies based on your delivery type, complications, and individual healing. Women over 40 benefit significantly from pelvic floor physical therapy assessment—a specialized therapist can evaluate your specific dysfunction and create a targeted recovery plan.
Red flags requiring immediate medical attention include: heavy bleeding, severe pain, fever, signs of infection, or worsening symptoms despite rest. Don’t push through concerning symptoms hoping they’ll resolve on their own.
C-section recovery requires additional considerations. Your abdominal incision needs adequate healing time before you engage core muscles intensively. Vaginal delivery, especially with tearing or episiotomy, requires careful progression to avoid straining healing tissues.
The Right Mindset for Sustainable Results
This is a marathon, not a sprint. Progress isn’t linear—you’ll have good days when everything feels stronger and setbacks when symptoms resurface. Both are normal parts of recovery.
Quality matters more than quantity in every movement. Five perfectly executed pelvic floor contractions deliver better results than twenty sloppy ones. Focus on feeling the correct muscles engage rather than rushing through repetitions.
Track improvements beyond the scale. Notice functional changes: Can you walk farther without discomfort? Do you leak less during exercise? Can you lift your baby without back pain? These real-world improvements matter more than any number.
What You’ll Need (Spoiler: Almost Nothing)
Comfortable clothing that doesn’t restrict your abdomen and a yoga mat or soft surface provide everything you need to start. Optional additions include resistance bands for progressive strengthening and a small pillow for support during certain positions.
Your most important tools are a quiet space for 12-25 minutes daily, your breath, and your commitment. This isn’t about expensive equipment or gym memberships—it’s about consistent, intentional practice that rebuilds strength from the inside out.
Phase 1: Weeks 1-4 – Gentle Reconnection Exercises

Diaphragmatic Breathing (The Most Powerful Starting Point)
Lie on your back with knees bent and feet flat. Place one hand on your chest and one on your belly. Inhale slowly through your nose, directing breath into your belly so the hand there rises while your chest stays relatively still. Exhale slowly through your mouth, feeling your belly fall and your pelvic floor gently lift.
This simple practice rebuilds the breath-pelvic floor connection that pregnancy disrupted. Practice 3-5 minutes, 2-3 times daily—during feeding time, before sleep, or whenever you have a quiet moment.
Why this exercise builds the foundation for everything else: It teaches your nervous system to coordinate diaphragm, core, and pelvic floor movement. Without this coordination, advanced exercises won’t deliver optimal results.
Pelvic Floor Awareness and Gentle Kegels
Identify your pelvic floor muscles by imagining you’re stopping urine flow (don’t actually do this during urination—it can create dysfunction). You should feel a lifting, tightening sensation without engaging your glutes, thighs, or holding your breath.
The proven 10-10-3 rule: Perform 10 quick squeezes (contract for 1-2 seconds, release completely), followed by 10 slow endurance holds (contract for 5-10 seconds, release for 10 seconds), three times daily.
Incorporate these exercises during feeding time or while rocking your baby. These small windows of time make consistency achievable without adding another task to your overwhelming schedule.
Pelvic Tilts and Cat-Cow Stretches
Pelvic tilts rebuild spinal mobility while gently engaging deep core muscles. Lie on your back with knees bent. Exhale as you tilt your pelvis, pressing your lower back into the floor and engaging your pelvic floor. Inhale to release. Perform 10-15 repetitions, moving slowly and breathing naturally.
Modified cat-cow on hands and knees promotes gentle spinal movement. Exhale as you round your back (cat), engaging pelvic floor and drawing belly in. Inhale as you arch your back gently (cow), allowing pelvic floor to release. Move slowly through 8-10 repetitions.
These movements reduce back pain, improve posture, and reconnect you with your core without the strain of traditional ab exercises. They’re gentle enough for early recovery but powerful enough to create meaningful change.
What to Avoid in Early Recovery
No crunches, planks, or high-impact activities during this phase. These exercises create excessive intra-abdominal pressure that overwhelms healing pelvic floor muscles. Avoid breath-holding during any movement—this increases pressure and interferes with proper muscle coordination.
Signs you’re pushing too hard: increased bleeding, pelvic pain, heaviness, or worsening leakage. When symptoms worsen, scale back intensity and rest. Your body is communicating its limits—listen carefully.
Phase 2: Weeks 5-8 – Building Functional Strength

Bridges with Pelvic Floor Integration
Bridges sculpt your glutes while strengthening pelvic support. Lie on your back with knees bent, feet hip-width apart. Exhale as you lift your hips, engaging your pelvic floor first, then glutes. Hold for 3-5 seconds, maintaining neutral spine. Inhale as you lower slowly. Perform 10-15 repetitions, 2-3 sets.
Progress by lifting one leg (single-leg bridge) or elevating feet on a step. Each progression challenges stability and builds strength that translates to real-world activities like climbing stairs or picking up your baby.
This exercise combats “mom butt”—the flat glutes many women develop postpartum—while creating the pelvic floor strength necessary for more advanced movements.
Wall Squats and Modified Squats
Wall squats provide the safest introduction to lower body strengthening. Stand with your back against a wall, feet hip-width apart. Slide down until thighs are parallel to the floor (or as far as comfortable). Engage your pelvic floor as you push back up. Perform 10-15 repetitions, working up to 3 sets.
Progress to freestanding squats when you can perform wall squats without pain or heaviness. Focus on form: knees tracking over toes, weight in heels, chest lifted, breathing coordinated with movement.
Squats build functional strength for lifting your baby, carrying groceries, and every daily activity that requires lower body power. They’re one of the most efficient exercises for rebuilding total body strength.
Standing Functional Movements
Step-ups mirror the movement of climbing stairs while building single-leg strength and balance. Step up onto a stable surface with one leg, engaging your pelvic floor and core as you lift. Step down slowly and repeat 10 times per leg.
Modified lunges (when ready) challenge stability and strength through a larger range of motion. Start with small movements, focusing on control rather than depth. Carrying exercises—holding light weights or your baby while walking—build the strength you need for daily life.
These functional movements prepare you for real-world activities, building confidence alongside physical strength.
Lifestyle Factors That Accelerate Your Results
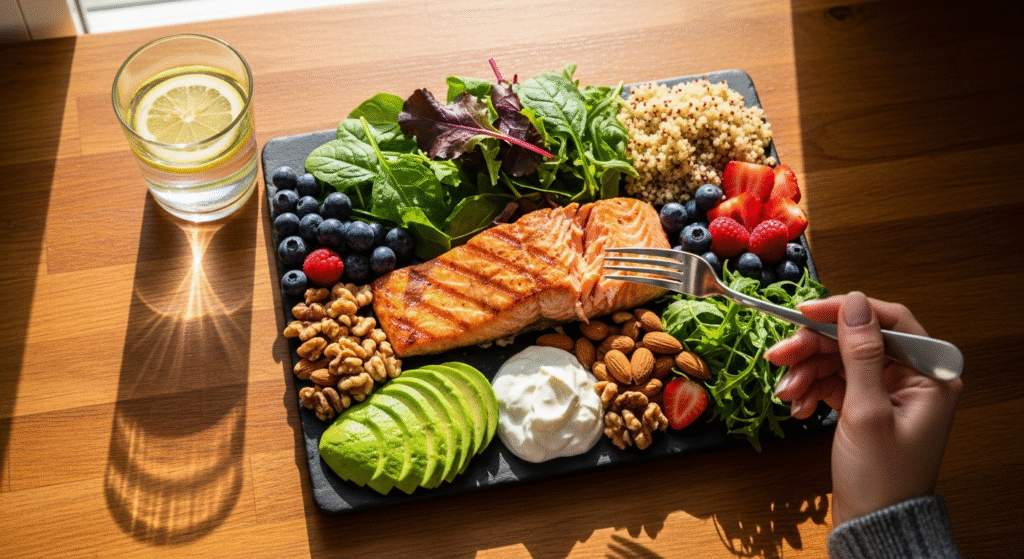
Nutrition for Tissue Repair and Hormone Balance
Protein requirements increase during postpartum recovery—aim for 0.8-1 gram per pound of body weight to support muscle rebuilding. Women over 40 need adequate protein to counteract age-related muscle loss while recovering from pregnancy.
Hydration affects tissue elasticity and healing. Drink at least 8-10 glasses of water daily, more if breastfeeding. Dehydration impairs collagen production and slows recovery.
Foods rich in vitamin C, zinc, and amino acids support collagen production: citrus fruits, berries, leafy greens, bone broth, wild-caught fish. Anti-inflammatory foods—omega-3 fatty acids, turmeric, ginger—reduce inflammation that interferes with healing.
Sleep, Stress, and Recovery
Rest isn’t lazy—it’s when healing happens. During sleep, your body produces growth hormone and repairs damaged tissues. With a newborn, quality matters more than quantity. Take naps when possible, even 20-minute power naps support recovery.
Stress hormones like cortisol create pelvic floor tension and interfere with healing. Practice short relaxation techniques: 5-minute guided meditations, gentle stretching, or simply sitting quietly with your breath.
These small practices compound into significant healing support when practiced consistently.
Posture and Daily Movement Patterns
How you hold your baby affects pelvic floor pressure. Bring your baby close to your body rather than holding them away from your center. Use a supportive carrier that distributes weight evenly.
Lift from your legs, not your back. Engage your pelvic floor before lifting anything heavy. Stand and sit with neutral spine alignment—imagine a string pulling the crown of your head toward the ceiling.
Transform everyday activities into strengthening opportunities. Engage your pelvic floor while washing dishes, folding laundry, or standing in line. These micro-practices build strength without requiring dedicated exercise time.
—
Your body deserves this intentional recovery. You’re not just healing from childbirth—you’re building a foundation of strength that will serve you for decades. Start with Phase 1 today, even if it’s just 5 minutes of diaphragmatic breathing. Small, consistent actions create powerful transformations. Your pelvic floor recovery journey begins now—and you have everything you need to succeed.